During a womens health appointment, firstly you will be made to feel at ease! You can expect a thorough discussion about your condition which will include taking a full medical history, discuss your symptoms and concerns related to this and sometimes discuss things more holistically around your whole health. You will also be asked whether you have tried any treatments before.
- Wear something comfortable, that you can move around in.
- Also something that you can get changed in and out of easily may be useful as well.
A physical examination will be required and this may mean looking at how you move and how your body is put together to see if larger themes may be playing a role to your concerns. This may involve assessment of your trunk, legs and arms. Even bladder and bowel concerns can be tied to your whole body.
Equally, this may also include checking your pelvic floor muscles (this is with your full consent). We are assessing for strength, co-ordination and function. Sometimes assessing organ function with visceral manipulation and possibly imaging tests like Ultrasounds.
It is important that you understand the ways in which the therapist might interact with you and your body and at any stage you can say ‘NO’ and ask for an exam to be ended at any point.
The therapist may include certain things in the appointment and give you things to do at home. Together, these may include:
Women's Health Treatments
- hands on treatment (manual techniques),
- Discuss some changes to the way that you eat/drink or urinate/defecate
- Stretching and exercises
- Breathing techniques
- Pelvic floor exercise
- Acupuncture
- Self massage
- Life style changes
- Give you handouts
This will all be to help you meet your goals.
It is essential to communicate openly and honestly with your therapist during the appointment. But remember the plan is for YOU! So please speak up if any parts of it are confusing or don’t seem possible for you in your current situation.
If you are in pain, we can help
or call 01889 881488
Jean, Erica & Charlotte will be happy to help
Olympic Bronze Medalist 1992 Barcelona
Women’s Health & MSK Physiotherapist

When I started working in the Staffordshire area I soon heard about Nicky Snazell and how she was an amazing holistic practitioner. That was me, a holistic physio who looked at people as a whole. I was intrigued. I wanted to find out a lot more about Nicky and her clinic.
Read on to follow Sandra’s story.
I was soul searching and thought why not just reach out to Nicky. She engaged with me immediately and I knew that the connection was there. The thought of having the opportunity to work in a clinic with such an amazing therapist as Nicky completely blew my mind!
On visiting the clinic and meeting Nicky and Alan face to face I thought I had come home. It was a perfect setting and felt like I had visited the clinic before, although of course I hadn't. All the staff were so welcoming and warming.
On watching Nicky treat some of her patients, I knew I had to work here. She treated patients completely differently to anything I’d witnessed before and it was clear that her dry needling skills were at an unbelievably high level.
Although I am bringing another skill to the clinic as a Women’s Health/ Pelvic Health physio, I do use acupuncture as a treatment modality on a daily basis and Nicky would be a phenomenal acupuncture and dry needling mentor! The training and education that she has shared worldwide is amazing and I wanted to have some of that, as part of her team, shared with me too.
I am naturally very competitive, always striving to be my best, never accepting the status quo. I thus have a strong need to learn and learn from the best, as only the best will do. That’s why joining the team at Nicky Snazell Clinic was so important to me.
"I am so glad to be welcomed on board. Thanks for having me, I am honoured."
If you are suffering with any pelvic floor problems, then you are not alone, as a third of women suffer with this at some point in their life. Don’t suffer unnecessarily. Help is at hand.

If you are in pain, we can help
or call 01889 881488
Jean, Erica & Charlotte will be happy to help
Women are not talking about their Pelvic Health enough. Perhaps it’s because they are too shy or too embarrassed to talk about it. Not discussing these openly can lead to a sense of isolation for those suffering with the symptoms of bladder or bowel incontinence, prolapse, sexual dysfunction or any other pelvic health condition.
Sadly, most people have no idea what Pelvic Health is and more importantly that real and effective help is available to women of all ages.
Read on to understand more about how a pelvic health specialist can help you.
If you have a sore knee, shoulder or back, you would probably have no hesitation to go to a therapist. If you can get yourself to think about Pelvic Health as just another type of problem that can be helped, then seeking that help will come naturally and without hesitation.
If you have a sore knee, shoulder or back, you would probably have no hesitation to go to a therapist. If you can get yourself to think about Pelvic Health as just another type of problem that can be helped, then seeking that help will come naturally and without hesitation.

Specialist pelvic health physiotherapy is probably not the first thought when people realise they need help because they start leaking with exercise (stress urinary incontinence), suffer vaginal prolapse or have an over active bladder. Yet there is robust evidence around pelvic health physiotherapy and it is recommended as the first line of treatment for a variety of pelvic health conditions. That’s why GP’s and Consultants refer to specialist pelvic health physiotherapists.
Even with such referrals, clients usually turn up and have no idea why they are here and how physio is going to help them. Thus, ever since qualifying in this specialism, I have been on a mission to educate and help make a difference to women’s lives.
We need to start to chat about bladders, bowels and vaginas and do this openly, without embarrassment. My main mission is to empower you to take control of your pelvic health as much as possible without the need for drugs or surgical intervention.
If you are suffering with any of these conditions, we can help. You can be confident that your concerns will be dealt with both sympathetically and confidentially.
If you are in pain, we can help
or call 01889 881488
Jean, Erica & Charlotte will be happy to help
There are various types of massage and often the most avoided is Deep Tissue, simply because the name is a bit scary and it sounds painful. But be under no illusion, Deep Tissue Massage opens pandora’s box to feeling in less pain, more flexible and healthier than you have in your life.
Find out more about how deep tissue massage can benefit you.
There are lots of different types of massage and each have their benefits and weaknesses.
Swedish
If we start with Swedish Massage, this is the softest variety and is wonderful for just wanting to feel pampered and relaxed. Therapeutcally, however, its benefits are marginal at best and what it does provide is short lived.
Sports Massage
This is a step up from Swedish and tends to be provided by therapists who are trained in human anatomy, so understand which muscles are most likely linked to a given problem, and can treat that accordingly. It’s generally a stronger type of treatment than Swedish and if the therapist is focussing on a localised problem, can cause pain that varies from uncomfortable to strong. There are two things to note here. First, resolving painful knots is obviously going to aggravate things and cause more short term pain but, and this is the kicker, the pain level will subside quickly as the problem is resolved in follow on massages.
Deep Tissue Massage
Sports massage can be highly effective in treating more superficial problems, but sometimes the techniques simply won’t get in far enough for deep seated problems. In such cases, the big guns need to brought out, so that the treatment can get in deep enough to be effective. At the same time, however, there are also relatively shallow problems that sports type massage could easily reach, but the added pressure used in deep tissue massage is way more effective.
That effectiveness, however, does come with more pain - for the first few treatments that is. Yes, it’s a bit of ‘no pain, no gain’, but for those willing to accept this, the gains are substantially greater and once gained, most are reluctant to lose them again. Put simply, a body regularly treated with deep tissue massage, will feel at a level above it has ever felt before.
(Interesting fact- In Germany, Doctors often prescribe a course of Deep Tissue Massage in preference to drugs as their first line of defence. Now why would they do that unless it really works?)
Emotional pain likes to hide out deep in the body, deep in a pit, so much so, it’s like an archaeological dig to find it. Such pain is caused throughout our life whenever our body experiences emotional trauma, responding by going tense, our fight or flight response. This shuts down oxygen to some muscles and viscera and that’s usually a time of intense anger or fear. Emotional notes, as well as physical pain are a physical manifestation of what our emotions are at that time, and unfortunately can become imprinted within our bodies and reside there, the cause long forgotten, locked in for years like unexploded land mines.
A deep tissue therapist can then unwittingly come along in search of deep tissue trigger points, the aim being to release physical pain and tension, only to be bombarded by a huge emotional release as the land mine explodes.
The good news is that this release is a vital step to a long term resolution of pain.
The deep trigger points can be treated with deep tissue massage, applying focussed pressure, encouraging the muscles and fascial tissue to relax, releasing toxins and improving oxygen flow. The latter is important as restricting the oxygen supply can upset the nerves and cause chronic super sensitivity within those nerves. The result of this is the birth of chronic painthat won’t ever go away.
When we release these trigger points, you must understand there is a lot of emotional baggage that can go with it. It thus helps if your therapist can also work with a healing ability and so heal the emotion as it erupts.
This why deep tissue massage is such a wonderful treatment, alongside deep seated physical release, you have a treatment for mental wellbeing.
In some situations, curing a deep seated, stubborn pain might need a finely focussed deep needling technique called GunnIMS, and in this we are blessed by having one of the very top practitioners in the UK at our clinic.
If this is something that calls to you, pick up the phone and let’s chat.
If you are in pain, we can help
or call 01889 881488
Jean, Erica & Charlotte will be happy to help
It’s all too easy to choose the first clinic you see listed or hear about. After all, they must surely all be same and it will save me a whole lot of time if I stick with this one, won’t it? Well, no, actually it won’t, any more than searching for a car with four wheels would be fine when you get offered a Ferrari and a Rolls Royce while you were thinking of something more like a Mini. Even a simple bit of refinement of your search, like ‘small 2 door car that can do at least 50 mpg’ would cut the list down massively.
Ok, this is a very simple example and one where most people are going to have a fairly good idea of what they want and don’t want.
But if you have never been to a private therapy clinic before, it’s not going to be so easy because you don’t have any idea of what you need to ask to help get you to the right place and more importantly stop you wasting your time or money on the wrong place.
Read on find out the three questions you must get answered before you make your choice.
The questions need to be for any clinic you consider, but we will answer them here for our clinic so that you get an appreciation of how expansive the questions are.
What should you need to find out first?
1. Can they help you by fixing your problem?
2. Do they have the expertise to sort out your particular problem? Can you trust them to do this?
3. Do they offer good value?
So firstly, can we help you?
Well, let’s start first with our name, ‘Nicky Snazell’s Wellness and Physiotherapy Clinic’. That actually tells you three things.
1. It’s a Physiotherapy Clinic. There are different types of physiotherapy specialism and our clinic focusses on your musculoskeletal frame, your joints, your spine, the nerves, muscles, tendons and ligaments that supply those joints, referred to as MSK Physiotherapy.
If you have a problem with any of those parts, anywhere in your body, from head to toe, then that we can help sort. Your problem may have resulted from a sports injury or from a simple trip, a major fall or just be part of having seen too many summers. If you are in pain or have restricted flexibility, we can help.
2. It’s a Wellness Clinic. Now there’s a good chance this will cause confusion because the term ‘wellness’ is so liberally and often misleadingly claimed. We haven’t got to ‘wellness rubbish collectors’ yet, but you get my drift.
Wellness to us has a very deep meaning of taking account of a clients’ inner health and not just their physical problem. For example, all too often there is a clear link between mind and body, yet this is overlooked.
Nicky Snazell (more on her shortly) after years of research, developed her own wellness criteria, looking for those conditions which would have an impact on both the problem itself and the best route to treat it. Her wellness model takes into account four key factors of lifestyle, mindset, fitness and diet, each scored on a simple traffic light basis of red, orange and green. What she found was that two clients, presenting with almost identical problems, but one with four red keys and the other with four green keys, needed very different treatments for success. In fact, a treatment which helped the four green key holder was contraindicated for the four red key holder. Without a deep understanding of wellness, this important differentiation could be completely missed, resulting in a client getting the wrong treatment, and apart from being painful, will potentially waste a lot of time and money.
3. The clinic has the owners name above the door. That’s a stamp of authority and recognition within her peer group. To you, a potential client, that means trust and confidence. Just as Rolls Royce won’t compromise their name with anything but the best, ‘Nicky Snazell’ over the door means no different.
It’s a personal reputation and it took many years to gain. In Nicky’s case after setting up Physiotherapy departments in both the NHS and private sectors, she started her own clinic and won the approval of several Consultant Surgeons who chose to consult at her clinic.
Nicky has written five books on Physiotherapy and Health, is currently writing her sixth, has consulted in Harley Street and been invited by over 30 radio stations across the USA to provide expert opinion on ways to help the opiate crisis without drugs. She has won awards from the UK based AACP, been a speaker at their conferences, presented on health internationally and awarded the first fellowship in the world to ISTOP, by it’s founder Professor Chan Gunn. Perhaps of most significance to you though is that many clients have travelled not only from every corner of the UK to seek Nicky’s help, but also from thousands of miles away from different countries and continents.
All of the above took dedication and years of hard work. Her stamp over the door of her clinic is her commitment to any client who enters the door that they will be provided the best treatment possible.
If you find another clinic with the owners name over the door, you know that the owner is similarly putting their reputation on the line and you should take confidence from this.
A great indicator of how much trust you can put in us is to ask others. Google reviews provide exactly that. Personally, I wouldn’t go near anyone, in any business, with a score below four out of five. Also, make sure a clinic has a lot of reviews before giving the score too much credence. The fact is everyone has a few friends to put in a nice word. Very few have hundreds. We have over 150 and our score is 4.9. Put another way, over 90% of our clients rate us 5 stars.
Second, do we have the expertise to help you with your particular problem?
It’s one thing to determine if a potential clinic can most likely help you. It’s another thing to establish if that clinic has the expertise and resource to help your specific problem.
There are perhaps the more obvious questions to ask such as ‘how many years’ experience do you have’ and ’have you treated this problem before’. Larger clinics will have more therapists and there will be a range of experience and different specialisms, thus one therapist could be much more suitable to you than others.
Now a completely different aspect of any clinic comes to the forefront. Does the clinic have a knowledgeable reception team who can determine who is going to be the best fit to your problem. Let’s face it, without this kind of help, your chances of doing the same are slim to none. It’s much better to be able to talk to a knowledgeable person up front. There are subtleties in here that only by talking do you get them resolved. For example, you might be very motivated by preventative help, so it would be better for you if your therapist thought the same way.
Another factor, most likely something that you would not have even thought of, yet very important, is the amount of in-house training, called CPD, that takes place. The benefits of this to you should be obvious – a team that constantly cross trains learns faster, broader and deeper.
You might then be surprised that many clinics don’t do this at all, it’s just hands to the pump treating clients.
Nicky Snazell, who has a strong drive to constantly learn and be ahead of the curve, makes sure that ongoing CPD is an integral part of her teams activity and CPD is a weekly event for every therapist.
One final factor which will make a lot of difference to your treatment success is how well equipped the clinic is. Nowadays there is a plethora of sophisticated equipment which can help a lot but that takes huge investment, which is why many clinics have very limited technology support.
At our clinic, constantly investing in new technology has always been part of our philosophy and on more than one occasion we have pioneered new technology. The real bonus to you, however, is that all this technology is made available to you at no extra cost. Make sure you ask the cost of technology with any clinic you may consider.
Third Question. Do we offer good value?
The answer to that question is very much dependent on what you value the most. For the majority, we find that clients want to be able to get on with their lives, doing what they love doing, whether it be enjoying sports, gardening, playing with the grandkids or just continuing to be able to positively contribute to society. Being in pain stops all of this, your life stops, and the value of your life falls off a cliff.
Poor health choices in the long term can lead to a permanently restricted lifestyle, a dependency on toxic drugs and maybe even surgery.
What value then to find a clinic that can provide a broad range of skills, a pioneering attitude to knowledge and technology introduction, a desire to provide proactive help to keep chronic pain at bay? Only you can make that decision based on your values.
Our clients are like family, and they feel confident and safe the moment they first walk through our door. Many want to pass the message on so that we may help others and we in return offer half price treatment for referring (rules apply) and we have a loyalty scheme that our clients love. When you add access to all our range of technology at no extra cost, and the very high level of skill and knowledge on site, plus these great ways to save on treatment cost, then value from us shifts massively in your favour.
Three questions you should have answered before you make your choice. Not easy to answer simply, as they provoke many considerations that need to be answered. This emphasises, however, the importance of getting it right to avoid wasting time and money, but most important of all the negative impact it will have on your life.
If you feel we might be a good fit for you and simply would like to know more, then give us a call. We have a very friendly team, Jean, Erica and Charlotte, who are there to help.
If you are in pain, we can help
or call 01889 881488
Jean, Erica & Charlotte will be happy to help
Most of us know deep down that a good massage helps alleviate pain, stress and anxiety, and helps promote flexibility and looking younger. Why is it then that most casually dismiss the benefits of an occasional rub, even though they may be needlessly suffering some, or even all of the above symptoms?
Read on to find out more about how massage could help you.
Massage is a pillar to physiotherapy, in fact physiotherapy started with four lady masseurs in the late 1800’s, who could see the benefits of hands-on therapy. Of course, physiotherapy has grown in capability massively since then, in line with our greater understanding of the physical body, in part due to vastly improved scanning technology. Rather than diminish the significance of massage, however, this increased knowledge has only served to amplify its benefits.
Thus, just as its founders recognised over 100 years ago, massage remains an essential tool in the physiotherapists toolbox. A well-trained therapist will use his or her hands not only to treat, but also diagnose, as they will be able to pick up tight muscles, knots and problems in connective tissue that would be totally invisible to even the most advanced scanning technology available today.
Massage is not just for the physical ailments, as it can equally help resolve locked in stress and anxiety, which resides in the stomach and gut. (Have you ever noticed when you are stressed or upset that you so often suffer an upset stomach? That mind-body link is so often overlooked and yet so important to overall wellness)
Physiotherapists make massage an integral part of their treatment to rejuvenate health for 7 reasons:
M is for movement of your connective tissue, allowing the layers to slide, rejuvenating cells, and giving a flexible youthful glow to the skin. Stimulating fibroblasts to make youthful collagen, keeping your skin soft and supple, looking younger.
A stands for Anti-Aging, accelerating blood flow, boosting circulation, oxygen and nutrients and invigorating your body’s vital systems enhancing longevity.
S signifies stress release, melting physical and mental anxiety, promoting wellness.
S for stimulation of the lymphatic system, crucial for detoxifying your body and boosting your immunity. We also use deep oscillation through our hands on technology that boosts stimulation.
A alleviation of pain, targeting and releasing sore trigger points and stretching out tight muscles
G denotes greater flexibility, stretching and loosening the muscles and joints, improving your range of motion.
E is for emotional balance, harmonizing your body and mind, elevating your mood, and fostering emotional resilience.
If you want to step into a physiotherapy session that embraces peace and vitality, then find someone like us that combines massage within physiotherapy.
Whether you are looking to relieve chronic pain, reduce stress or speed up the rehab of a sports injury, come over to our physiotherapy sanctuary.
Ready to embrace a healthier, relaxed, more vibrant you and let the healing begin?
Give us a call to find out more.
If you are in pain, we can help
or call 01889 881488
Jean, Erica & Charlotte will be happy to help
Have you ever been haunted by a knife-like pain down your leg? Not just down your leg but in every aspect of your life. Making the simplest of tasks, like putting your socks on, impossible.
Imagine a pain that shadows you from the moment you get up and even haunts you at night, stopping you from sleeping.
You are not alone. Nearly half of us have suffered this at some time in our lives.
To learn more about sciatica and how to treat it, read on
It’s called sciatica and its root cause is a modern lifestyle of poor posture and weak muscles.
The videos explain what sciatic is and how the structure of the spine is vulnerable.
The sciatic nerve is a big nerve running from the back to the feet. Nerves, any nerves in your body in fact, don’t like to be squeezed and tell you quickly about this by causing pain. Typical causes of nerve compression are:
• Spinal discs act as cushions between the bony vertebrae, allowing movement and keeping the discs nicely spaced apart, allowing nerves to move freely and without pain. If those discs get compressed sufficiently, nerve compression and pain can result.
• Powerful back muscles can react to this nerve compression and go into spasm, increasing nerve compression and pain.
• Each pair of spinal vertebrae have joints between them to help control movement, called facet joints. These joints get worn with age and trauma and can eventually cause further nerve irritation.
• Our bodies are covered in a layer of connective tissue below the skin (imagine bubble wrap) and this tissue can become less flexible as we age, also leading to possible nerve irritation.
These underlying causes are nearly always quickly reversible with the correct lifestyle adjustments, adherence to exercise prescriptions and hands on physiotherapy. In more severe chronic cases, especially with locked in muscle spasm, specific dry needling may be required. There’s no one size fits all solution. A thorough assessment and treatment plan will be the most effective and fastest solution.
If your physiotherapist has any concerns, she or he can touch base with your doctor for bloods, x-rays or a scan.
Off the shelf pain meds, like anti-inflammatory with paracetamol can help. Your pharmacist can advise if its safe for you to take them with preexisting conditions or other meds.
or call 01889 881488
Jean, Erica & Charlotte will be happy to help
Breaking Point
Breaking Point is my sixth book, currently being written and hopefully in the shops by autumn. It’s atransformational fiction – solving & healing a spiritual murder mystery.
This story embarks on a journey of discovery, revealing how hidden traumas lodged deep within the body can be unearthed and transformed through innovative treatments.
Drawing upon the wisdom of over 100,000 orthodox treatments, this narrative entwines a spiritual essence, sharing my unique perspective on healing.
Through the compelling lives of fictional characters, I explain the process of identifying and addressing the root cause of your pain points with this distinctive healing approach.
I also have a book group on my Facebook pagewhere I release early drafts of ‘Breaking Point’ to seek constructive input. If you feel you would like to contribute and join my group, go to Facebook and search for ‘Nicky Snazell’ then request being a friend. Once you are accepted, you can ask to join the group.
If you would like to read the prologue to ‘Breaking Point’ then read on.
Breaking Point Prologue
Dear Reader,
Imagine you and I have time travelled together. We are standing together in the most beautiful garden on a balmy summers day, rose borders as far as the eye can see. The most immaculately trimmed lawns. Breathtaking old trees creaking in a gentle breeze, emitting wispy shadows as the sun weaves through the leaves. Gnarled, majestic Oaks to regal Ashes to elegant Silver Birch. In the near distance an iridescent lake with a shimmering green blue hue. It seemed to be a balmy early summer kind of day with fluffy white clouds and the sun shining through. I look down to see I am wearing a very pretty but faded long grey dress, a beautifully ironed crispy white apron with lace around the edges and old scuffed shoes.
You’ve noticed your clothes have changed too, haven’t you?
There is a rug spread out on the lawn and on it a simple basket full of sandwiches, cakes and homemade lemonade. There are three children close by. I know them as mine. Edward, my youngest at six, is playing with his box of alphabet bricks and chuckling to himself. Despite his health issues and missing a lot of school, he keeps learning as we teach him at home with the help of Nanny Nicole and Lady Jane, while I am kept busy housekeeping and cooking.
Edward loves playing and giggling with little Miss Penelope and she will be carried across soon to crawl on his rug to fill our day with joy.
His handsome father, Gwyn, the butler, ensures both his and Edwards little heart remains strong, swimming daily in the stately home pool. Sadly they share the same weak heart condition, caused by a genetic problem but also having personality’s overspilling with joy and loving kindness.
The sun is shining off Ted’s golden locks and I smiled at his little suntanned knees messing up his hidden slice of cake. I can hear the thump of a ball being thrown between his taller, short tempered and clever older brother John, who is ten and his strong minded but caring freckled- faced older sister Dorothy, who is eight. She attends the local school and helps with the chores. John is quite a handful and clearly getting irritated at his sister’s poor attempts at catching. He struggles to entertain his younger sister and brother but shines in his own right, bound for a successful career with his brilliant mind and boarding school education. Lord Charles is very kindly sending our eldest John to boarding school to gain a superb education. I am very proud.
As I look down, I see that Edward had mis-spelt ‘lof u’ with his wooden blocks. I spell it out again, ‘I love you too.’
Dear Reader, could you ask John and Dot to keep an eye on Ted as Nanny hasn’t arrived yet and I need a rest before I return to the house to prepare the vegetables for dinner and serve the family afternoon tea and cakes.
I stretch out, loosen my large white apron and have a snooze in the suns warm rays.
My rest is shattered, I awake to the screech of brakes and a tragic scene before my eyes. It feels as if everything has shifted, changed. I sense a deep fear, a dreadful rolling sensation in my stomach.
Ahead of me, I see a still, lifeless little boy, my Edward, just by the bend in the road which weaves down from the elegant stately home. No, no, no I scream. My beautiful child, I love him more than life itself. As I run to his motionless, still body I tell myself he that he must be asleep and he will wake up. My boy, my loving kind gentle, six year oldangel. His familiar little pale arms, outstretched. His curly, soft blonde hair and innocent cherub face with such long eyelashes over his closed eyes.
I had constantly dreaded the day he may collapse due to his heart condition, but nothing had prepared me for this.
Reader, can I take your hand for strength. Can you see this aura of blinding golden light around Edward?
I look down on his long dirty white socks, clean on this morning, his favourite little scruffy shirt, his torn teddy bear and his wooden cubes scattered.
There is something hauntingly familiar about this scene. As if I have been here before.
I know he’s not just asleep, a mother knows when her child is not breathing and dead. Yet I do not feel disconnected, as his shimmering soul is still here.
In my head I hear the words; “Mummy I can’t leave you.”
I'm suddenly aware of distant urgent shouts. I glance across towards the lake, as the dream shifts to a shimmering old vintage car, an exquisite red. I feel myself floating towards the car and as I get closer, I can see the water is starting to rise up inside the car. Fortunately, the car is not deep in the water but only three figures appear to be moving. Lady Jane, Lord James and Lord Charles, all screaming and crashing around as Lord James got his shoulder against the windscreen. Something feels very wrong, I can’tsense the presence of my Gwyn. I get closer, I gasp and tighten my grip on your hand, as I see that the driver, my darling husband, my soul mate, is slumped over the wheel echoing the stillness of our son.
I want to scream but there’s no voice inside me.
My children John and Dorothy were already by the car. The gardener, cap in hand, running in wellies, just shouts at me in terror.
I hear Dorothy start to scream as she spots her father.
I look around and the prettiest petit lady, Nicole, wearing her Nannies uniform and again an old fashioned starched white apron, runs towards me saying hold Penny, Lady Janes daughter. This toddler in a beautiful white dress and ringlets adores Edward. Nicole is sobbing as she rushes back to Ted’s lifeless body.
As I turn around to glance through tears at my tiny boy, hugging Penny tight, I see that a shimmering light surrounds him and is glowing brighter, an amazing golden glow. It stays there, then a ghost like image of my little body sits up and his cherub like, tear stained face looks towards me and says “you're next.”
“You too will be killed Mummy unless I stay with you and together we can save another soul. I will protect you, for I’m your guardian Angel and will always be in your heart, never far away and I shall pass over with you into your next life.”
I see this glow, this faint outline of my son, move over me and in me and I feel a deep sense of love and connection. The sense of deep loss goes. Just the grief for his physical presence remains as a dagger like pain. I feel his protection, love, and an eternal bond that transcends physical existence.
I wake up and I'm back in my bedroom again in 2024, damp with perspiration, bed clothes on the floor, my eyes wet with tears and my throat dry from screaming.
It’s nothing new to me to have dreams about past lives, but this recent reoccurring dream is now every night. It is getting tedious.
I know something is a foot.
Do you ever dream like this dear reader?
Can you join me in unravelling this mystery of who took the lives of this son and father and who now threatens mine?
If I may ask, are you happy to help me with this dilemma?
Would you come on a healing journey with me, to peer through the lens of my characters?
I was born with a secret gift beyond healing, a kind of telepathy that connects me to those both present and past, or rather passed. A sixth sense. At times conveying strong messages through dreams and visions.
I must say, I have never had such a repetitive dream. I was nearly reaching breaking point, on the brink of despair with this unrelenting nightmare returning night after night. Especially at such a profoundly inconvenient time, as I had been writing a book about the ramifications of the Pandemic and the surge for virtual medical consults. It appears destinyhad spoken and told me to rip that book up and rewrite a new version. The universe had chosen a different narrative for me to explore with you. It seems I am to write a different book so I must trust the time must be right to do this.
Blackie, my rescue cat was visibly irked. As a streetwise cat, he saw me as a soft touch, perceiving my soft hearted nature and had soon exchanged my heated greenhouse with its cozy cat basket for the house and bed.
His sleep had been disturbed yet again and he needed to express his frustration, so he scratched up the bed and carpet again.
Then went straight under the duvet.
I gave myself a shake which sent Blackie flying into an unintended orbit. I told myself to get a grip, to get showered, grab a cup of earl grey tea and get to my clinic, as there would be a list of folks waiting for me with hidden pain to seek out and kill.
or call 01889 881488
Jean, Erica & Charlotte will be happy to help
Radial shockwave provides a non-invasive gentle treatment, designed to alleviate pain and speed up recovery from injury. Despite what the name might suggest, it does not involve any kind of electrical shock treatment. Instead, it sends low energy pressure waves into damaged tissues to stimulate the body’s natural repair process, speeding up recovery and reducing inflammation.
A common concern is that treatment will be painful and the answer is reassuringly no. In fact, most clients describe the sensation as being similar to a gentle tapping on the skin.
This non-invasive treatment is very effective in treating problems such as:
- Plantar Fasciitis
- Calcified tendonitis
- Chronic tendon problems (tendinopathies)
- Achilles
- Knee
- Elbow
- Shoulder - Muscle tightness
- Legs
- Buttocks
- Spine
- Arms
We have made shockwave a standard part of the treatment we offer and have kept to our ethos of providing the best value treatment we could by providing shockwave at no extra charge. This is something we still do today and our clients love the fact that is an integral part of our hands on treatment capability.
or call 01889 881488
Committed to provide the best treatment value to you
Our clients love shockwave and we also found that they liked a device called a V-ACTOR, which is a very powerful vibrational therapy tool, the power coming from the shockwave internals. Understandably our V-ACTOR has been sought after but only having one on site has restricted access at times.
Our major focus, however, has been on the shockwave treatment and over the years as demand grew we added more shockwave machines, eventually having four.
Top Quality Treatment. Available to you at no extra cost
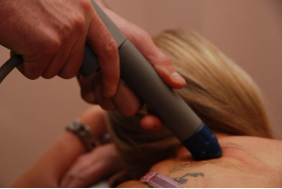
But our ethos remains the same – we want to provide the best treatment we can and that means the best hands on treatment, and for us that has to include both shockwave and vibrational therapy. Thus, we have taken the decision to add two more high quality shockwaves and both include the much loved V-ACTOR vibrational therapy. They are already on site and are available to you at no extra cost should you need it.
Having six shockwaves on site is perhaps a sign of our commitment to provide the best treatment value to you.
Jean, Erica & Charlotte will be happy to help
or call 01889 881488
You may have heard of gait analysis, you may even have visited your local running shop and had someone check your running out before buying the latest running shoe, but not all running gait analysis is equal and here’s why!
What if I told you that gait analysis is about more than just pronation and supination of the foot!
It's quite a bit more in fact.
or call 01889 881488
Footwear can play a big role in how your body reacts to the forces of running, but researchers have shown that some of the biggest injury risk factors are linked to your running form.
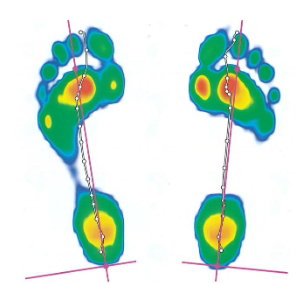
Understanding your gait for analysis
Improving your running form takes a rigorous process looking at the movements of the entire body. Our biomechanics team use `video gait analysis combined with industry leading Footscan plantar pressure data to distinguish between normal and pathological gait. This technology has been utilised in more than 3,000 scientific studies, trusted by state-of-the-art movement labs and elite sports teams worldwide.
It can also help us to make informed decisions on how best to manage your injury, be it through bespoke rehabilitation plans, running technique and coaching advice or custom orthoses.
Using Footscan we can design bespoke orthoses to aid with injury rehabilitation and performance, the same ones used by countless elite marathoners and footballers, should there be a need for them.
Aside from injury management, we also use our gait lab to help assess running technique with a view to improving running economy and performance. We can even predict overuse injury risk which is a leading cause of injuries in runners and military personnel.

From the moment you contact the ground to the moment you push off, your stride pattern speaks volumes about your injury risk and running economy, as such by analysing movement patterns and detailed data about your gait biomechanics we can really start to understand a lot more about how you could potentially move more efficiently and improve your running economy.
So, whether you are training for a marathon, or embarking on your couch to 5k this spring, we can help you solve those niggling injuries, or even unpick the lock to your next personal best!
